Breast Conservation Surgery & Sentinel Node Biopsy
The standard of care for Early Breast Cancer
Introduction
Breast Conservation Surgery & Sentinel Node Biopsy has been the standard of care for more than twenty years; with local control rates and overall survival being equivalent to Mastectomy. With recent advances in imaging techniques such as MR Mammography and the development of Breast Oncoplasty techniques, the overall results have further improved. Moreover with advances in Nuclear Medicine such as Sentinel Node Biopsy; we now also talk about conservative surgery for the axilla, thus limiting the post-operative complications of axillary dissection.
A case of Breast Conservation Surgery & Sentinel Node Biopsy
A 46 year old pre-menopausal female presented to our Institute with a recently noticed lump in left breast. On clinical examination there was a 2×2 cm size well defined lump in upper outer quadrant of left breast, with no significant palpable axillary lymphadenopathy. Digital mammogram done elsewhere showed a dense breast with a diffuse suspicious opacity in left breast. Fine needle cytology done outside suggested a papillary lesion. In view of high index of suspicion of malignancy we performed MR Mammogram, which showed a well-defined lesion in left breast upper outer quadrant along with two other suspicious lesions in close proximity to the main tumor. MR characteristics were highly suspicious for malignancy. There were however no significant axillary lymph nodes seen on MR. Ultrasound Guided trucut biopsy from the lump was positive for Ductal carcinoma. Metastatic workup (Chest X Ray, Ultrasonography of abdomen and whole body bone scan) were unremarkable.
Treatment Approach for Breast Conservation Surgery & Sentinel Node Biopsy
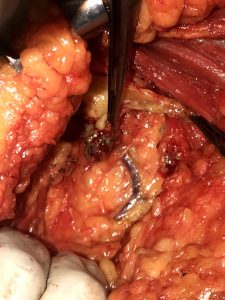
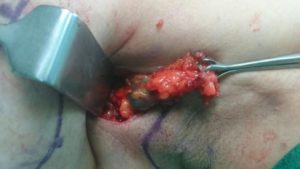
Although there were multiple lumps in left breast, in view of multifocal involvement limited to single quadrant with no significant axillary lymph nodes; the patient and family were counselled regarding the option of Breast Conservative Surgery and Sentinel Node Biopsy. The patient was subjected to breast scintigraphy on the day of surgery after injecting radioactive Tc99 nano colloid in retroareolar region of left breast. Gamma scan was performed in nuclear medicine department after 2 1/2 hour of injection; which showed uptake in two lymph nodes along anterior axillary fold. Patient was then shifted to the operation theatre. The sentinel lymph node were dissected by axillary incision and all suspicious axillary lymph nodes dissected were sent for frozen section analyses; which revealed absence of axillary lymph node metastases. Further axillary clearance was therefore not performed done.
A wide local excision of breast lump was done with a surgical margin of 1 cm circumferentially. The specimen was oriented and sent for frozen section confirmation of margins. The tumor bed was marked with surgical clips to aid in adjuvant radiation therapy planning. The defect created after removal of lump was reconstructed by breast oncoplasty by transposition and suturing of adjacent breast parenchyma into the defect (Breast Oncoplasty by Volume Displacement).
Discussion
Breast conservation surgery is currently the standard of care for treatment of early breast cancer with equivalent local controls and overall survival comparable to those with mastectomy. Most women with small breast lumps, therefore do not need to undergo mastectomy, i.e. complete removal of breast resulting in better cosmetic and psychological outcomes. Breast Conservation can even be offered to selected women with locally advanced breast cancers who have excellent response to pre-operative chemotherapy. MR Mammography helps in better selection of patients suitable for conservative surgery.
Patients with no palpable axillary lymph nodes or negative axilla on imaging can be subjected to sentinel node biopsy in order to look for suspicious hot nodes on scintigraphy, and therefore identify patients harboring metastatic lymph nodes which would require complete axillary dissection. In patients with negative sentinel lymph node on scintigraphy and frozen section; a full axillary lymph node clearance can be safely avoided with equivalent surgical and oncologic outcomes. Moreover, avoiding complete axillary dissection decreases significantly the chance of develop post-operative arm swelling and lymphedema which sometimes adversely affects long term functional outcomes and quality of life of patient.

These days after breast conservation, oncoplasty techniques and other local myocutaneous and fascio-cutaneous flaps are applied to reconstruct the defect. Compared to primary suturing of breast tissue these techniques give a better cosmetic outcome and near normal creation of the breast mound.
Dr Ashish Goel is the Breast Conservation Surgery & Sentinel Node Biopsy

